I was 28 the first time I had a full-body flare bad enough that I called in sick to work. My hands were swollen, my wrists ached from the inside out, and I sat on the bathroom floor at 6 a.m. trying to remember whether I had already taken my methotrexate that week. I grabbed the ibuprofen from the cabinet out of instinct, then put it back. My rheumatologist had told me twice to be careful layering NSAIDs on top of an immunosuppressant and I had ignored her twice. I was not going to do it a third time. What I did instead, out of desperation more than strategy, was reach for the tube of Biofreeze Pain Relief Cream that had been sitting untouched in my medicine cabinet for two months. It did not fix the flare. Nothing fixes a flare fast. But it took enough edge off that I could get dressed, get to my car, and get to work. That was enough.
Topical analgesics like Biofreeze are genuinely underused by younger arthritis patients. Most of us come into this disease assuming topicals are for gym soreness or old people with bad knees, not for someone in their 20s or 30s with autoimmune joint disease. But when your medication options are already maxed out, or when you cannot afford another NSAID day on your stomach lining, or when you just need something to get you through a Tuesday, knowing how to use a topical correctly makes a real difference. The word "correctly" matters here. Most people apply too much, in the wrong direction, at the wrong time, over skin that should not have it. This guide fixes that.
Already in a flare and need relief now? This is what I keep in my cabinet.
Biofreeze Pain Relief Cream 3oz uses pharmaceutical-grade menthol to interrupt pain signals at the nerve level. No NSAIDs, no systemic side effects. Works on wrists, knees, hips, shoulders, and ankles.
Amazon Check Today's Price on Amazon →Step 1: Recognize the Flare Early
The first skill is learning to catch a flare before it peaks, because topicals work better when the inflammation is building rather than fully erupted. The classic early signals: a joint that feels warmer than it should when you touch it with the back of your hand, visible puffiness around a knuckle or ankle that was not there the night before, and morning stiffness that is not resolving within 30 minutes of getting up and moving around. That 30-minute mark matters. Normal people get a little stiff when they first wake up. Inflammatory arthritis stiffness hangs around for an hour or more and often gets worse before it gets better.
Other early signals I have learned to recognize: fatigue that feels different from regular tiredness (more like a heaviness that sits in your joints specifically), a slight burning sensation in the joint at rest, and an increase in ambient pain that you cannot attribute to overuse. When I notice two or more of these, I treat it like the beginning of a flare, not something to push through. Catching it early means my tools, including Biofreeze, actually have room to help.
Step 2: Think Before Reaching for Ibuprofen
If you are on methotrexate, leflunomide, or a biologic like adalimumab or etanercept, your relationship with NSAIDs is more complicated than it was before your diagnosis. NSAIDs reduce inflammation, but they also stress the stomach lining and kidneys, and many disease-modifying drugs are already doing work in those same organ systems. This is not a reason to never take ibuprofen or naproxen. It is a reason to not make them your automatic first move every time a flare starts.
A topical analgesic like Biofreeze gives you a non-systemic option. The active ingredient, menthol at 4%, works via the gate-control mechanism, essentially flooding the sensory nerve pathways with a cold stimulus that competes with and partially blocks pain signals. It does not reduce underlying inflammation the way an NSAID does, but for the functional goal of getting through the next few hours, that distinction matters less than you might think. Save the NSAID for when you actually need it.
Step 3: Prepare the Skin Correctly
Before you apply anything, check the skin over the affected joint. Wash the area with mild soap and water and pat completely dry. This matters for two reasons: menthol absorbs more evenly through clean, dry skin, and broken or irritated skin dramatically increases absorption in ways that can cause burning or sensitization. Do not apply Biofreeze over broken skin, open wounds, a rash, psoriatic plaques that have cracked, or any area where you have recently applied a topical corticosteroid. The corticosteroid thins the skin barrier and changes how subsequent topicals penetrate. If you have used a steroid cream on that joint in the past 24 hours, skip the Biofreeze on that spot and apply it to adjacent muscle groups instead.
Also: do not apply immediately after a hot shower. Your pores are more open and the cooling sensation will feel uncomfortably intense, plus absorption will be uneven. Wait 10-15 minutes after showering.
Step 4: Apply in a Thin Layer, in the Right Direction
Most people squeeze out too much. A thin, even layer is all you need, roughly the size of your thumbnail for a wrist, and maybe twice that for a knee. Thicker is not more effective. The menthol can only penetrate so deep and so fast, and a glob of cream sitting on top of your skin just wastes product.
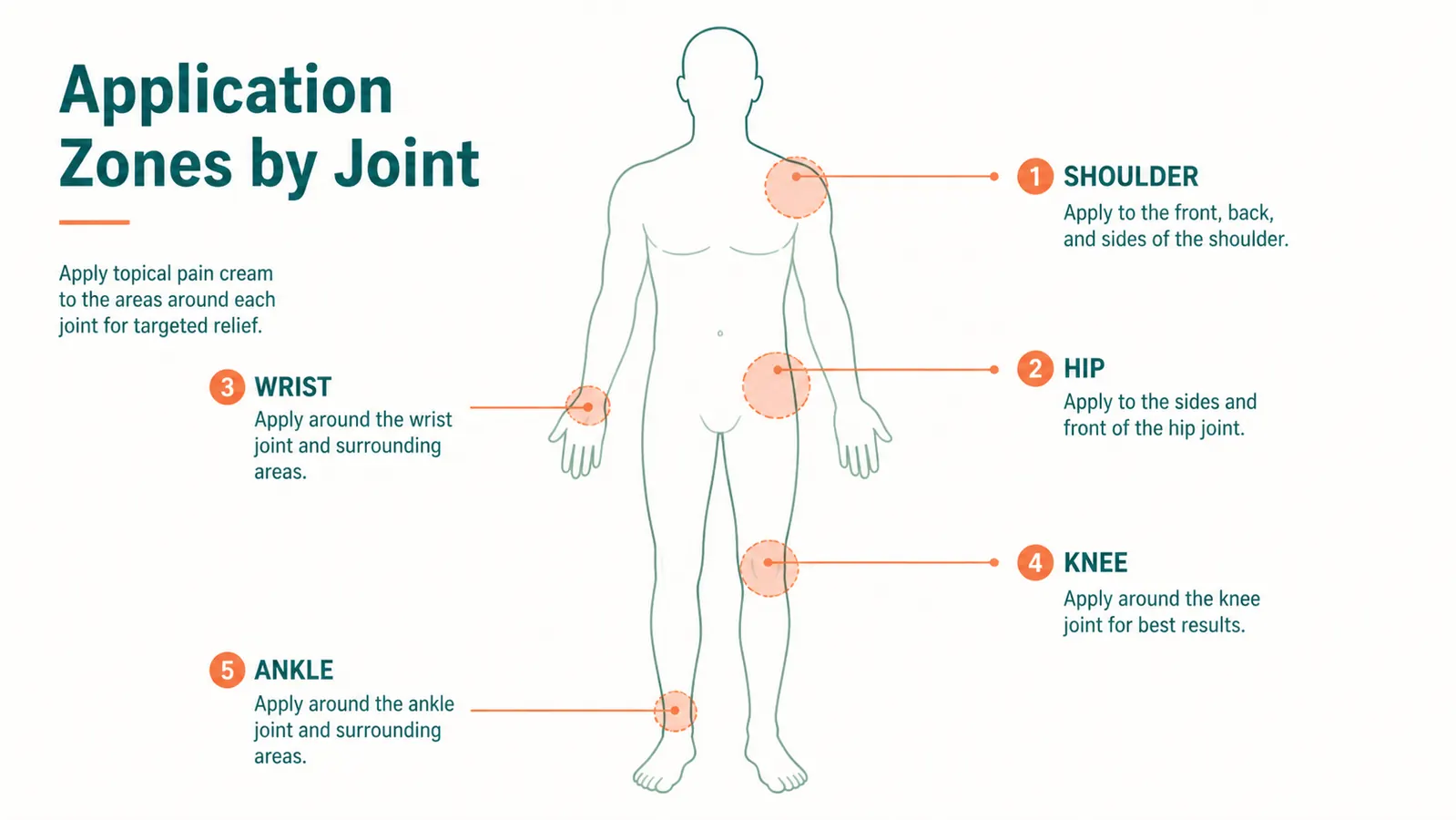
Direction matters more than most instructions admit. Apply the cream in long strokes that follow the direction of the underlying muscle or tendon, not in a circular motion over the joint capsule itself. For the wrist, that means stroking up the forearm toward the elbow along the flexor and extensor tendons. For the knee, stroke up and down the quadriceps tendon above the kneecap and the patellar tendon below it. For the shoulder, work along the deltoid and into the upper trapezius. The goal is to get the menthol into the periarticular soft tissue, not just sitting on top of bony prominences where there is less tissue to absorb it. Rub it in gently, do not massage aggressively.
Wash your hands immediately after unless you are applying to your hands directly, in which case let it absorb for at least 5 minutes before touching your face, eyes, or mucous membranes.
A glob of cream on top of your joint does not work better than a thin layer. It just leaves you sticky and wastes half the tube.
Step 5: Wait the Full Activation Window
Set a timer. The menthol needs time to work. You will feel a light cooling sensation within 60-90 seconds of applying, but that is not the same as the analgesic effect starting. The actual pain-signal interruption builds over 5-8 minutes and plateaus around the 8-10 minute mark. Most people apply the cream, feel the initial coolness, decide it is not working, and immediately do something that disrupts the process, either rubbing the area more, covering it with something warm, or getting up to move around.
Sit still for 8-10 minutes. Let the menthol finish absorbing. This sounds simple but it is the single step most people skip, and it is the single step that most affects whether the topical works. If you apply and immediately go wash dishes or type on a keyboard, you are washing off or friction-rubbing away half the dose before it has had time to penetrate.
Step 6: Pair With a TENS Unit If You Have One
Biofreeze and a TENS unit can work together during a flare, but there is a specific rule you need to follow: never place TENS electrodes over an area where you have just applied a menthol topical. The topical changes the impedance of the skin, which can cause uneven electrical stimulation, skin irritation, or in some cases burns under the electrode pads. Place the TENS pads on a different site, typically one joint position away from where you applied the cream.
The practical version of this: if you applied Biofreeze to your wrist joint, place the TENS electrodes on your forearm mid-muscle belly, at least 3-4 inches above or below the cream site. The TENS works on the gate-control mechanism from a different input point. You are effectively hitting the pain pathway from two different positions at once, which many people with chronic arthritis find significantly more effective than either tool alone. For a deeper look at how TENS units work for joint pain and how to use them, see our guide on TENS units vs heating pads for joint pain.
Step 7: Reapply on Schedule, Not on Instinct
Biofreeze's active effect lasts roughly 3-4 hours at the application site. The instructions say maximum 4 applications per day. Follow both of those. Do not reapply at the 1.5-hour mark just because the cooling sensation has faded, because the cooling and the analgesic effect are not the same thing, and the analgesic may still be working even when you no longer feel the cold.
Set a calendar reminder or phone alarm for 3 hours after each application if you are managing a bad flare day at work. Doing it on schedule is more effective than waiting until the pain spikes back up and then reapplying reactively. If you notice skin redness, a rash, or itching at the site after any application, stop using it on that skin area. Some people develop a contact sensitivity to menthol, and continued use on sensitized skin makes it worse.
Step 8: Protect Your Posture and Range of Motion During the Flare
There is a specific kind of bad advice that circulates in fitness and even some physical therapy spaces: that you should stretch through the pain to prevent stiffness. During an active flare, this is the wrong call. Inflamed synovial tissue is more vulnerable to micro-damage when stressed, and aggressive stretching can extend a flare that would have resolved in 3-4 days into one that goes 7-10. The menthol from the Biofreeze may reduce the perceived pain enough that a joint feels more mobile than it actually is, and this is where people push too hard and pay for it the next day.
What you want instead is gentle, active range of motion, meaning you move through the comfortable portion of a joint's range without forcing into resistance. For the wrist, this means slow circles that stop at the first sign of resistance, not circles that push through it. For the knee, this means walking at a pace where the joint feels supported, not hiking stairs to prove you are fine. Topical relief is a tool for function, not a green light to train.
Step 9: Track the Flare in Writing
This step is the one that most changed how my rheumatologist manages my treatment. When you show up to a quarterly appointment and tell your doctor you had some bad weeks, that information is nearly useless clinically. When you show up with a notebook that says flare started Thursday the 14th, right wrist and left ankle, started applying Biofreeze at 7 a.m., pain at 6/10, resolved mostly by day 4, that is actionable data.
Keep a simple flare log. Date started. Joints involved. Peak pain score on a 1-10 scale. What tools you used (topical, TENS, heat, rest, NSAID) and whether they helped. How long until you could do your normal daily tasks. If you are on a biologic or DMARD, note whether the flare started close to an injection or dosing window. All of this helps your rheumatologist see patterns, adjust timing of doses, add or remove medications, and understand whether your current regimen is actually working. A few sentences every day during a flare takes two minutes and is worth far more than you would expect. For more context on how I use Biofreeze as part of a broader flare management routine, my full review at Biofreeze for Rheumatoid Arthritis Pain covers the longer picture.
Step 10: Know When to Call Your Rheumatologist
Topicals have a real place in flare management but they do not replace medical care and there are specific situations where you need to stop self-managing and call your doctor. Call your rheumatologist or go to urgent care if:
You develop a fever above 100.4 F alongside joint pain. Fever plus joint pain is a red flag for septic arthritis, which is a medical emergency that requires IV antibiotics and can permanently damage a joint in 24-48 hours if untreated. Immunosuppressed patients are at higher risk for septic arthritis than the general population and should not wait it out.
A single joint becomes extremely hot, red, and swollen in a way that is dramatically out of proportion to your other symptoms. One hot red joint when everything else is relatively calm is classic septic arthritis presentation, not a standard inflammatory flare. Do not put Biofreeze on it and go to sleep.
A flare has lasted more than 7 days without improvement. At that point your current medication regimen may need to be adjusted, a short course of oral prednisone may be warranted, or there may be a secondary cause triggering the prolonged flare that your rheumatologist needs to investigate.
Knowing these limits is not pessimistic. It is what makes every other step in this guide actually safe to follow. If you are curious how other people with RA have used Biofreeze through a multi-week flare, the first-person account in Biofreeze Got Me Through My RA Flare is worth reading before your next bad stretch.
What Else Helps Alongside Topical Relief
Biofreeze is most useful as part of a layered approach rather than a standalone strategy. The tools that work well alongside it during a flare: a heating pad on adjacent muscle groups (not directly over the inflamed joint capsule itself, which tends to feel worse with heat when actively flaring), a TENS unit as described in step 6, compression sleeves or gloves to reduce the sense of internal pressure in the joint, and rest with the affected limb supported in a neutral position. Elevation helps with swelling in lower extremity joints. Ice packs can help acutely, though many people with autoimmune arthritis find that sustained cold aggravates rather than helps, so follow what your own body tells you.
What does not help: deep-tissue massage directly over an inflamed joint, hot baths when a joint is actively red and hot, alcohol (it is a vasodilator and tends to worsen next-day inflammation), and most importantly, trying to white-knuckle through a full work schedule on no rest. One good half-day of rest early in a flare often shortens the total duration more than pushing through two full days of work and paying for it all week.
One good half-day of rest early in a flare often shortens the total duration more than white-knuckling through two full days of work.
If you are still deciding whether Biofreeze is worth keeping in your toolkit, the detailed breakdown of how it compares to other topical approaches is in our piece on Biofreeze for rheumatoid arthritis pain. And if you want the honest version of what this cream does and does not do for autoimmune joint pain specifically, the personal flare story is a better read than any manufacturer page.
Keep a tube within reach. On a bad flare morning, you will not regret it.
Biofreeze Pain Relief Cream 3oz is what I use every time a flare starts climbing. Menthol-based, no systemic side effects, works in under 10 minutes. The 3oz tube fits in a work bag or desk drawer.
Amazon Check Today's Price on Amazon →